Among the top contributing authors of the new groundbreaking study of Ellen T. Roche et al. entitled “A light-reflecting balloon catheter for atraumatic tissue defect repair,” in Science Translational Medicine, is 31 year-old Greek researcher from Harvard Biodesign Lab, Panagiotis (Panos) Polygerinos.
Polygerinos is currently an Assistant Professor of Engineering with the Ira. A. Fulton School of Engineering at Arizona State University.
The Greek innovator describes below the main function of an ultraviolet (UV) light-equipped catheter, which is able to repair holes in the heart using a biodegradable adhesive patch.
Can you tell us about the novelty of this study?

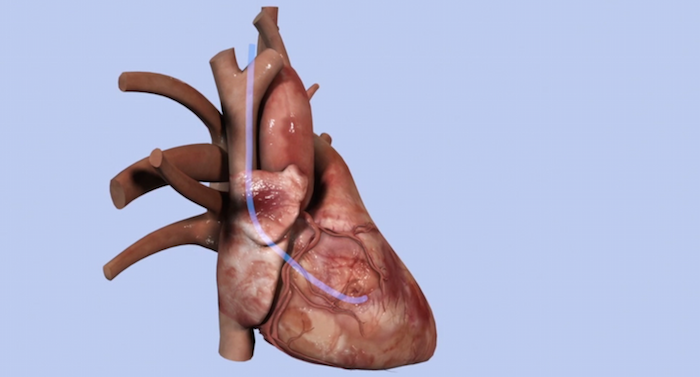
Scientists, surgeons and engineers with different backgrounds worked together to offer patients and clinicians a minimally invasive approach with which the stitching of tissues for closing small defects in the body during surgery may be avoided in the future. The new catheter, which is equipped with a UV light and a biodegradable adhesive patch can be inserted through a vein to reach the patient’s heart.
How does the UV light-equipped catheter work?
While in the patient’s heart, the catheter releases an adhesive patch and two balloons, one on each side of the hole. The main function of these two balloons is to apply pressure from both sides of the heart wall securing the patch in place. The next step is to turn on the catheter’s UV light that is transmitted through an optical fiber cable to the distal balloon. After the light reflects off the balloons’ reflective interior it activates a UV light sensitive glue which attaches the patch to the heart wall.
What follows the activation of the glue?
Both balloons are then deflated and the catheter is removed leaving behind the patch, which serves as a biodegradable scaffold permitting normal tissue to eventually grow over it.
What are the potential broader implications of such a device in the future?
Our study not only demonstrates a potential noninvasive cure of heart hole defects, but it also paves the way for the management of gastrointestinal diseases such as ulcers and hernias. This approach could ultimately lead to the avoidance of invasive surgical procedures and sutures and simplifies the cure of otherwise currently complicated medical conditions.
Dr. Polygerinos, who currently runs the “ASU Bio-Inspired Mechatronics Lab,” received his Bachelor’s degree in Mechanical Engineering from the Technological Educational Institute of Crete in Greece. After he completed his M.S. degree in Mechatronics and Ph.D. in Mechanical Engineering (medical robotics) in King’s College London, London, U.K., he joined as a postdoctoral fellow at the Harvard Biodesign Lab, directed by Prof. Conor Walsh and the Wyss Institute for Biologically Inspired Engineering at Harvard University.
While a Wyss postdoctoral fellow of Technology Development at Wyss Institute, Polygerinos took part in several scientific projects developing new soft wearable assistive and medical technologies.

You can watch a video explaining the study of Ellen T. Roche et al. below:
See all the latest news from Greece and the world at Greekreporter.com. Contact our newsroom to report an update or send your story, photos and videos. Follow GR on Google News and subscribe here to our daily email!



